AsianScientist (Oct. 31, 2021) – Mental health conditions often fly under the radar as symptoms vary and are not always obvious. Whether misunderstood or readily dismissed, the hidden epidemic of mental health issues has grown even more prevalent during the pandemic, even leading to increased suicide rates in places like Japan.
In Singapore, the Institute of Mental Health found that 13 percent of over 1000 participants reported symptoms of anxiety or depression during the pandemic, though a lack of baseline statistics made pre- and post-COVID-19 comparisons difficult.
While COVID-19 may have exacerbated the issue, the global mental health toll has snowballed due to longstanding neglect and inequities. Over 264 million people worldwide suffer from depression, and millions more live with other mental health conditions, making it clear that increased help, support and comprehension are paramount.
To promote healthy lives, the United Nations’ Sustainable Development Agenda has identified mental health disorders as a strategic priority to be addressed by 2030. This timely focus on mental healthcare looks at the inaccessibility of sufficient services, compounded by persisting social stigma and an overall lack of data around these illnesses.
Digital mental health could change this narrative, overcoming barriers of cost, geographic distance and patient distrust. But it will require more than just the thousands of wellness apps already available on the market; instead, continued innovation is the key to eliciting evident changes in quality of life.
As we near the end of yet another pandemic year, we envision what the mental healthcare system of the future might look like, driven by advances in key technologies.
1. Providing direct and continued support
Given the discomfort and shame that can surround mental health disorders, individuals may be more willing to disclose personal and emotional information with chatbots rather than with other people. These virtual companions would serve as an objective platform to encourage sufferers to seek help, making mental health support accessible at any time for a broader audience.
Through conversations and storytelling, chatbots are being developed to detect users’ moods based on the narratives they share. These virtual agents can then direct individuals to relevant clinical resources or guide them to reflect on their experiences—leading to better emotional regulation and psychological well-being.
Besides hesitancy over seeking out mental healthcare services, major barriers to access include geographic distance and the scarcity of healthcare specialists in both far-flung areas and densely populated communities. Computerized cognitive behavioral therapy can bridge these gaps, either powered by artificial intelligence agents or assisted by clinicians.
By leveraging the interactive nature of digital media, multi-week programs containing self-help modules could gradually steer participants away from distorted thinking patterns often associated with depression and anxiety. As low-intensity talk sessions, this form of therapy could encourage people to continue receiving care and develop healthier habits.
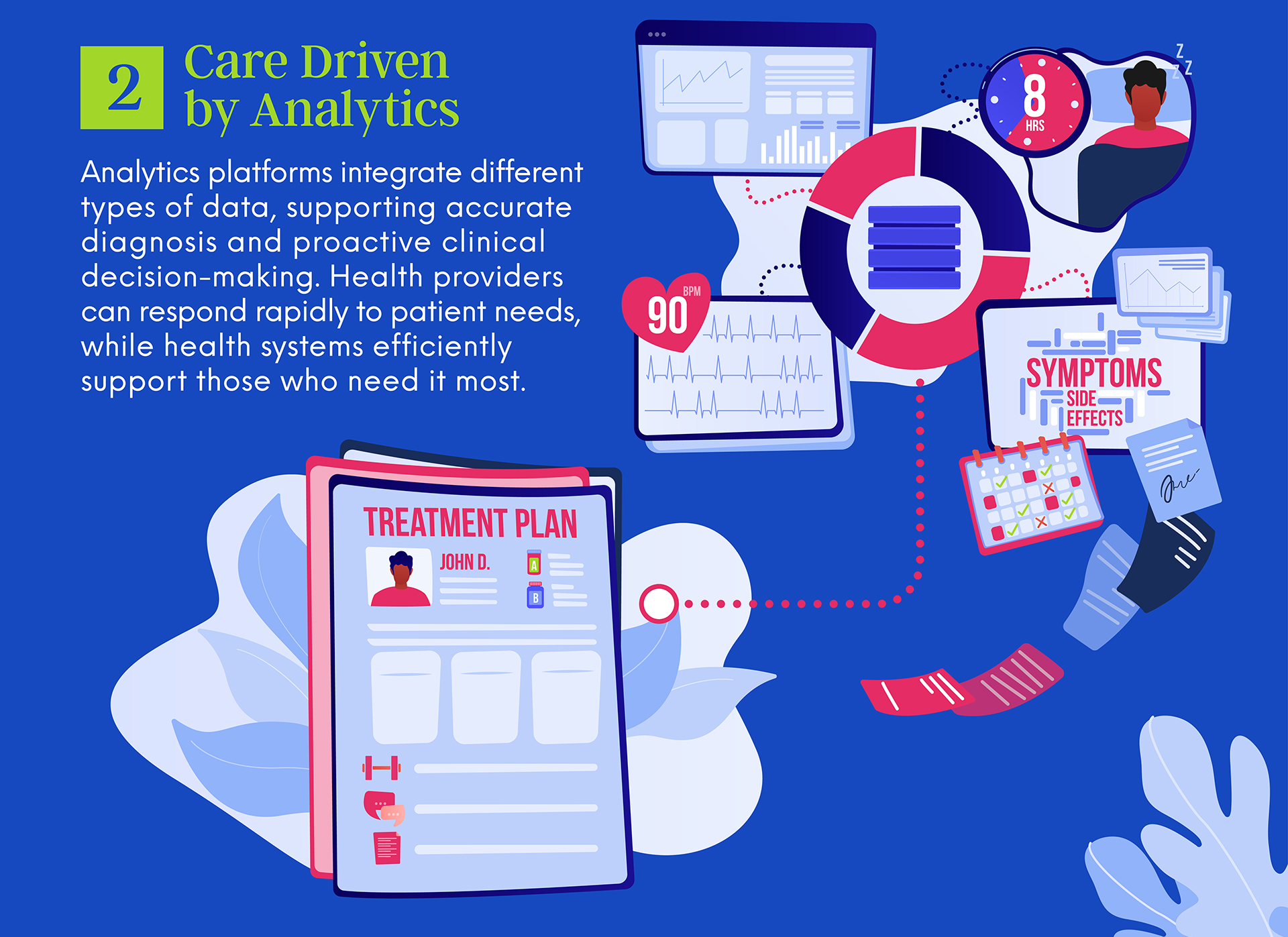
2. Delivering personalized mental health interventions
As mental health analytics advance, clinical care choices can similarly be enhanced with a personalized touch. Artificial intelligence-powered tools can combine physical data like heart rate as well as behavioral data like social media activity. Given the diversity of symptoms that can arise for various mental illnesses, such data can help tailor care to individual patient experiences.
Digital monitoring tools also complement the analytics platforms, with mobile apps like CureApp in Japan tracking behaviors like smoking for nicotine addiction patients. Wellness or journaling apps, combined with natural language processing models that extract key ideas from text, add an extra dimension for doctors to consider when diagnosing and assessing support options.
Together, the data from both home and clinical visits feed into the analytics platforms to paint a more complete picture of patient needs and treatment responses. With this back-and-forth mechanism enabled by analytics, doctors are equipped with up-to-date information about their patients. This would enable more personalized and adaptable treatment, meeting varying mental health needs even in between clinical visits.
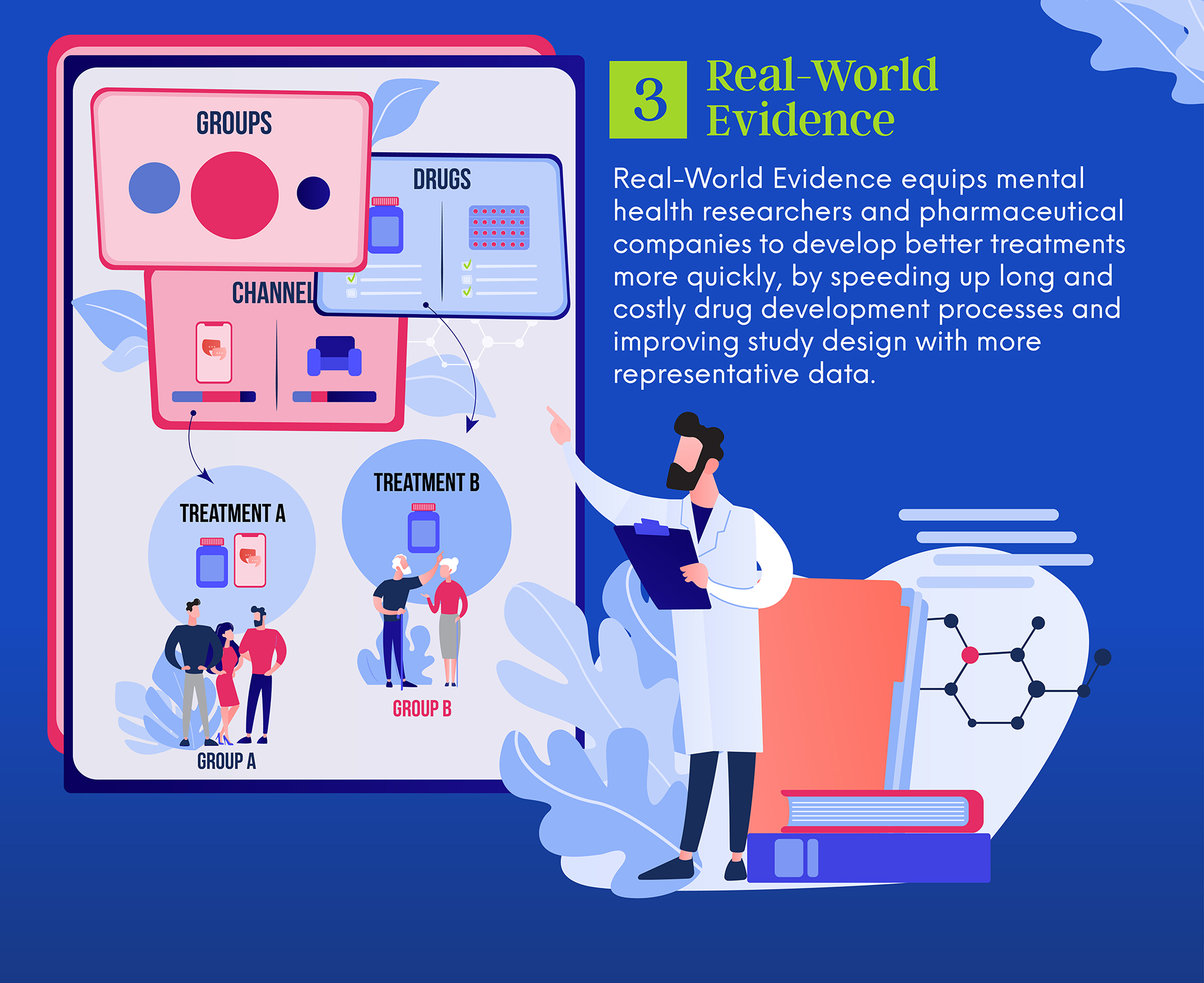
3. Drawing nuanced insights from real-world evidence
Given the different factors that can influence mental health status, research can often be confounded by data that has not been captured or has not yet generated meaningful insights when recorded.
To support both psychiatric research and clinical practice with relevant mental health data, clinical management systems provide a detailed picture on patient histories, including medical examinations and adherence to treatment regimens.
On a larger scale, the databases also collate important epidemiological data on the burden of mental health disorders in communities. Data security is also vital to managing these sensitive records, building trust and creating an environment where patients feel safe and empowered.
Through data analytics tools like health tech company Holmusk’s NeuroBlu platform, researchers can extract insights from real-world behavioral health data. The statistical analysis tools and interactive visualizations are key to building an extensive evidence stream, ranging from external stressors to drug side effects.
Such in-depth records on patient conditions help life science and healthcare partners refine study designs and develop more effective drugs for diverse needs.
By enabling a stronger link between research and innovation as well as clinical practice, real-world evidence can establish a stronger data-driven foundation for a responsive and integrated mental healthcare system.
While these digital solutions are exciting, none of them individually are the answer to solving mental health problems. Instead, they stand to form the core of a radically different mental healthcare system, if backed by sufficient digital infrastructure and clinical expertise.
In line with this, the World Economic Forum’s Global Governance Toolkit for Digital Mental Health provides useful guidelines for vetting the quality of these technologies. These holistic standards cover often overlooked socially responsive attributes, urging careful evaluation of the technologies involved.
When digital mental healthcare is not just effective but ethical and equitable, a future with improved personal welfare and healthier communities will no longer be an elusive dream.

Asian Scientist Magazine is a media partner of Holmusk.
———
Copyright: Asian Scientist Magazine; Illustration: Ajun Chuah/Asian Scientist Magazine.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.