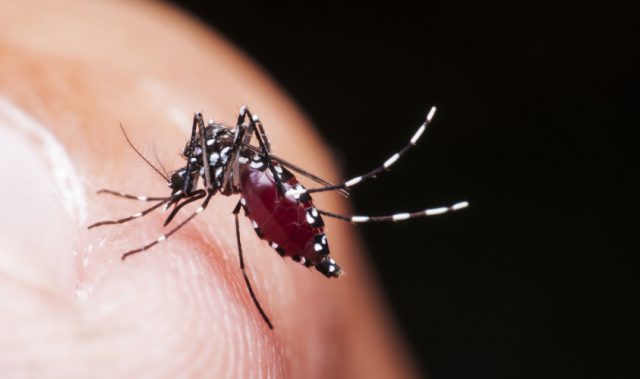
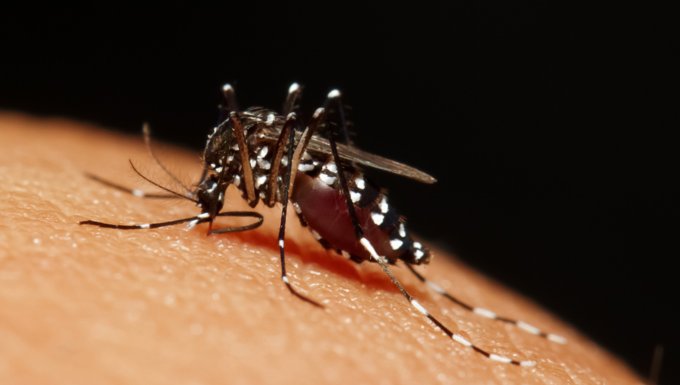
AsianScientist (Sep. 16, 2015) – Dengue, a mosquito-borne virus that infects some 400 million people every year, afflicts patients with fever, rash, and muscle pain. Most recover fully, but some go on to develop dengue hemorrhagic fever, a more severe condition characterized by vascular leakage—the loss of plasma through leaky blood vessel walls. Without proper fluid replacement, patients can die from systemic shock caused by low blood volume.
Dengue viruses are classified into four distinct but related serotypes. A first infection provides lifelong immunity against that specific serotype, but only partial immunity against the other three. Patients experiencing secondary or subsequent infections with a different serotype are more likely to develop severe dengue.
This is thought to be due to an overactive but ineffective immune response—antibodies specific to the first serotype do not completely neutralize the new one, and in fact allow the virus to more easily infect immune cells. The resulting high viral loads trigger a ‘cytokine storm’—the over-production of inflammatory cytokines that then makes blood vessel walls become too leaky.
In a study published in Science Translational Medicine, scientists led by Professor Paul Young at the University of Queensland report a crucial role for a viral protein, called non-structural protein 1 or NS1, in the development of vascular leakage. This is the first time that a viral protein has been directly linked to blood vessel permeability, and hence to the development of severe dengue.
Of the ten proteins that the dengue virus genome encodes, NS1 is the only one that is secreted into the bloodstream. Epidemiological evidence suggests that patients with severe dengue also have higher levels of NS1 in their bloodstreams, but its function remained unknown. Ms. Naphak Modhiran, a PhD student in Professor Young’s group and the first author of the paper, told Asian Scientist Magazine that this convinced the researchers to examine the potential role of NS1 in disease.
“The mysterious nature of NS1 made the work more challenging and interesting,” she said.
The researchers found that treating immune cells with NS1 activated them and induced them to produce inflammatory cytokines. Monolayers of endothelial cells (similar to those that make up the walls of blood vessels) became more permeable when the researchers treated them with NS1.
The team found that NS1 binds to Toll-like receptor 4 (TLR4), a molecule on the surface of immune cells known for recognizing and activating inflammatory responses against bacterial lipopolysaccharide (LPS), a component of bacterial cell membranes.
When the researchers blocked TLR4 signaling with either a TLR4 antagonist or an anti-TLR4 antibody, the effect of NS1 on immune and endothelial cells was lost. Further experiments also showed that treatment with a TLR4 antagonist alleviated vascular leakage in a mouse model of dengue infection.
This suggests that NS1 may act in manner similar to bacterial toxins such as LPS—by binding TLR4 and activating the production of inflammatory cytokines that then triggers vascular leakage. Indeed, the hallmarks of LPS-induced bacterial sepsis—increased production of inflammatory cytokines, increased vascular permeability, and subsequent septic shock—are uncannily similar to dengue-induced shock.
Scientists are now interested in developing anti-dengue vaccines and drugs that target the NS1/TLR4 interaction. In a separate study published in the same issue of Science Translational Medicine, researchers led by Professor Eva Harris at the University of California, Berkeley found that immunizing mice with small amounts of NS1 protected them against subsequent lethal dengue infection. Such a vaccine, if developed, could prevent at-risk patients from progressing to severe dengue.
The findings also suggest that TLR4 antagonists, which have been tested (so far unsuccessfully) in clinical trials against bacterial sepsis, could potentially be repurposed to treat dengue. But there are many challenges to such a strategy, says Modhiran.
One is the need to determine the best window of opportunity for treatment, such that the immune system is not thrown too far off balance by the blockade of TLR4 signaling. The Australian team is now carrying out preclinical studies to evaluate potential drug candidates, in the hope of securing support for future clinical trials.
The article can be found at: Modhiran et al. (2015) Dengue Virus NS1 Protein Activates Cells via Toll-Like Receptor 4 and Disrupts Endothelial Cell Monolayer Integrity.
———
Copyright: Asian Scientist Magazine; Photo: Shutterstock.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.