AsianScientist (Nov. 16, 2016) – Since Dengvaxia, the world’s first dengue vaccine, was rolled out, there have been mixed reactions as to its efficacy. Asian Scientist Magazine speaks to Dr. Ng Su-Peing, global medical head of Sanofi Pasteur, to find out more about Dengvaxia and how it fits into dengue control efforts in Singapore and beyond.
- How does the Dengvaxia vaccine work?
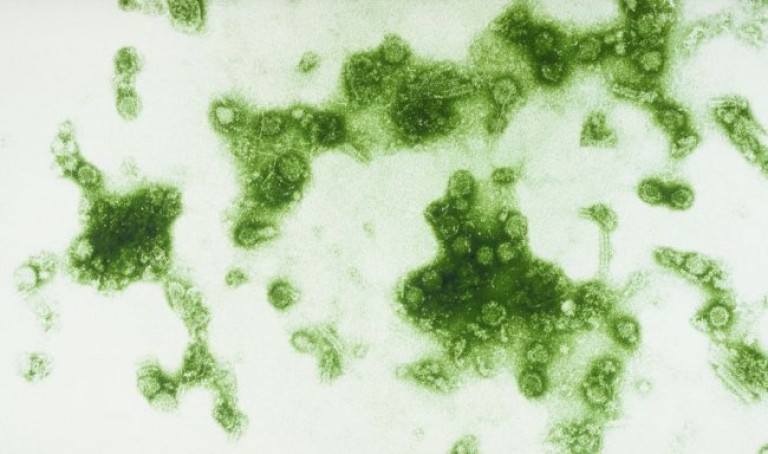
Dengue is a mosquito-borne viral disease that has spread to most tropical and many subtropical areas. The disease is caused by four closely-related viruses, the dengue virus types 1-4. There are no specific treatments for dengue, and until the Sanofi Pasteur dengue vaccine, prevention was primarily limited to vector control measures.
The vaccine is designed to induce an immune response against each of the four dengue viruses, but not to cause disease. The immune response results in antibodies capable of fighting dengue infections.
- How does vaccination fit in into a wider dengue control strategy in endemic, tropical countries such as Singapore?
Until the development of the Sanofi Pasteur vaccine, there was no vaccine or clinical preventive measure against dengue available to healthcare professionals. Currently, there remains no specific medical treatment for the disease.
Traditional means of controlling outbreaks of the disease have been through elimination of breeding areas, fogging operations with anti-mosquito spray and increased inspections of potential breeding grounds by organizations such as the Singapore National Environment Agency. With the Aedes mosquito preferring to breed in clean, stagnant water, about two thirds of breeding sites are found in homes.
As the government continues to conduct its dengue prevention measures in the community, the new vaccine could provide an additional means for individuals in Singapore to supplement their efforts to avoid dengue infection. In other dengue-endemic countries where the dengue burden is higher than Singapore, routine and catch-up mass vaccination programs could help achieve a greater impact in terms of more rapidly reducing the disease burden. The Philippines and Brazil are two countries that have introduced public vaccination programs in specific areas or populations.
- Several countries across the Asia Pacific and the rest of the world are adopting Dengvaxia. How is Sanofi Pasteur assisting in the smooth nationwide deployment of the vaccines in these countries?
In 2009, Sanofi Pasteur built a dedicated production facility for the dengue vaccine in order to secure adequate supply of quality product in a timely manner to countries upon approval. This facility has a production capacity of 100 million doses per year; this means one billion doses in ten years. Deliveries to meet orders for both public programs in the Philippines and Brazil and demand from private patients in other endemic countries where the vaccine has been registered have proceeded smoothly, and as anticipated.
- How is Sanofi Pasteur helping poorer countries with vaccine costs?
Sanofi Pasteur is committed to offering a fair and equitable price for the vaccine that is sustainable for both the company and the governments where the vaccine is approved. Price for the vaccine in public programs will be determined once agreement has been reached on the nature of the dengue immunization program needed in the country to address its dengue burden.
To date, in all the countries where we have conducted cost-effectiveness analyses, Dengvaxia has been shown to be cost-effective or even cost-saving, based on the WHO criteria for cost-effectiveness which accounts for GDP of the country and, hence, affordability. These analyses incorporate current country-specific burden of disease, dengue epidemiology and overall cost burden of dengue, as well as the documented clinical profile of the vaccine.
- In the Philippines, there has been public resistance to vaccination with Dengvaxia over fears that the vaccine could cause side effects. What kind of side effects are these and does protection against dengue outweigh their dangers?
The Philippines Department of Health has confirmed the Dengue School-Based Immunization program being implemented in the National Capital Region, Central Luzon, and Calabarzon will continue and not stop as claimed by some groups. No safety concerns related to vaccination were observed after analyzing data from over 20,000 clinical trial participants from 9-60 years of age who had received the vaccine.
The most common side effects were headache, muscle ache, injection site pain, tiredness, feeling unwell and fever. These effects were mild to moderate in severity, lasted up to three days, and resolved on their own. The side effects described by participants who received the vaccine were generally comparable with those described by study participants who had received placebo control.
- Dengvaxia displayed limited efficacy in serotype 2 dengue sufferers, and in children under the age of nine, a high-risk group. Could you briefly explain in layman terms why this is so?
As dengue is a complex disease, the virus interacts in different ways with the human immune system, and different serotypes can co-circulate or change in prominence from year to year in dengue-endemic countries. The combined data from Asia and Latin America studies in the 9-16 year old age group showed that approximately two out of three vaccines were protected against dengue of any severity caused by any of the four serotypes.
Furthermore, efficacy was significant for each serotype with higher protection against serotypes 3 and 4 seen compared with serotypes 1 and 2. Importantly, vaccine efficacy against all four serotypes also contributes to the ability of the vaccine to prevent eight out of ten dengue hospitalizations and nine out of ten severe dengue cases in the first 25 months following the first dose.
Some efficacy was observed in clinical study participants below nine years of age. However, until more data is gathered as part of long-term evaluations, the overall benefit of vaccinating children under nine against dengue remains to be determined. As the nine and above age group represents the majority of dengue cases worldwide as identified by national surveillance systems in several dengue-endemic countries, and up to 90 percent of dengue cases in some endemic areas, a vaccine indicated for a targeted population of nine years and older has the potential to significantly impact dengue disease in high-burden countries.


———
Copyright: Asian Scientist Magazine; Photo: Shutterstock.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.