AsianScientist (May 11, 2020) – Using a CRISPR/Cas9-based system, researchers at the University of Tokyo have screened nearly 20,000 genes to identify a new regulator of a key protein linked to Alzheimer’s disease. Their findings have been published in FASEB Journal.
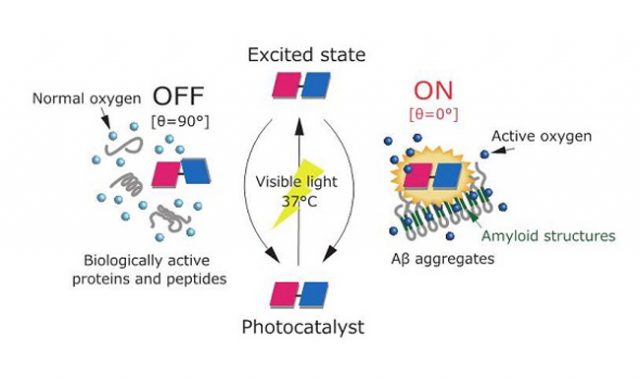
The exact causes of Alzheimer’s disease remain unknown, but one of the most popular theories focuses on a protein called amyloid beta. The aggregation—or clumping together—and depositing amyloid beta and another protein called tau are a signature of Alzheimer’s disease.
To identify genes that regulate the levels of amyloid beta, the team used CRISPR/Cas9 to systematically delete 87,897 guide RNA sequences, covering a total of 19,150 genes. They then selected cells that showed higher or lower levels of amyloid beta, using next generation sequencing to identify 13 possible genes responsible for the altered levels of amyloid beta.
“We believe this is the first time anyone has used this CRISPR/Cas9 genetic screening technique to look for changes in amyloid beta production,” said Dr. Yukiko Hori, a co-first author on the research paper.
By testing each of the 13 candidate genes, the researchers narrowed their focus down to calcium and integrin-binding protein 1 (CIB1), showing that cells without functional CIB1 genes produced abnormally high levels of amyloid beta protein.
“Nobody knows why the deposition of amyloid beta occurs in Alzheimer’s disease patients’ brains, but we think a starting point of the process could be CIB1,” said Professor Taisuke Tomita, leader of the research lab that performed the study.
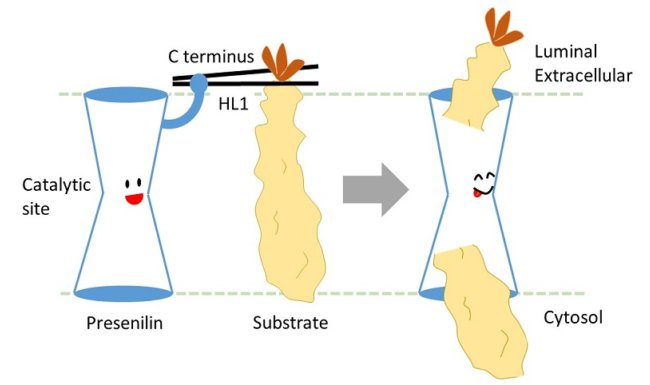
Gamma secretase is an enzyme that is required to process amyloid beta precursors to the final amyloid beta protein. It is usually found inside the cell but moves to the cell membrane after processing amyloid beta. In healthy cells, CIB1 is not directly involved with processing amyloid beta, but stays attached to gamma secretase both inside cells and at the cell membrane. In cells without CIB1, gamma secretase spends more time inside the cell and does not move to the membrane.
“Our results show that regulating the location of CIB1 and gamma secretase could be a new target for Alzhemier’s disease therapy,” said Hori.
Convinced by their cellular experiments, the research team then decided to search directly for changes in the amount of CIB1 in the brains of Alzheimer’s disease patients. The patient data they examined comes from a long-term project based in the US called the Religious Orders Study and Memory and Aging Project (ROSMAP). The project tracks the health of volunteers who are all professional religious leaders (nuns, priests, brothers) and agree to donate their organs for research after their death.
People diagnosed with early-stage Alzheimer’s disease had lower levels of CIB1 in their brains than healthy people. Paradoxically, people diagnosed with late-stage Alzheimer’s disease had higher-than-healthy levels of CIB1.
“We cannot say for certain why CIB1 is increased in late-stage Alzheimer’s disease. What is important is that in both the early and late stages of Alzheimer’s disease, something is abnormal about the regulation of CIB1,” said Tomita.
Future research will uncover more details about the role of CIB1 in the cellular processes that lead to unhealthy levels of amyloid beta and Alzheimer’s disease. Researchers also plan to use their CRISPR/Cas9 screening technique to search for new genes that affect the other major Alzheimer’s disease protein, tau.
The article can be found at: Chiu et al. (2020) Identification of Calcium and Integrin‐binding Protein 1 as a Novel Regulator of Production of Amyloid β Peptide Using CRISPR/Cas9‐based Screening system.
———
Source: University of Tokyo; Photo: Shutterstock.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.