AsianScientist (Jul 14, 2014) – Scientists are now one step closer to a drug that could treat dementia and memory loss. A research team has discovered that reactive astrocytes, commonly observed in Alzheimer’s patients, aberrantly and abundantly produce the chief inhibitory neurotransmitter GABA, causing impairment in synaptic transmission, plasticity and memory. This discovery opens a new avenues for the development of new drugs to treat Alzheimer’s and other related diseases.
The study led by Dr. C. Justin Lee at Korea Institute of Science and Technology (KIST) and Dr. Kim Daesoo Kim from Korea Advanced Institute of Science and Technology (KAIST) has been published in the journal Nature Medicine.
Currently, there are only symptomatic treatments for Alzheimer’s disease, the most common cause of dementia. In Alzheimer’s disease, brain cells are damaged and destroyed, leading to devastating memory loss. It is reported that one in eight Americans aged 65 or over have Alzheimer’s disease. In 2011, 7,600 elderly people with dementia lost their way back home and became homeless in Korea. To date, there has been no clear understanding of the mechanisms underlying dementia in Alzheimer’s disease. So far, neuronal death is the only proposed mechanism available in scientific literature.
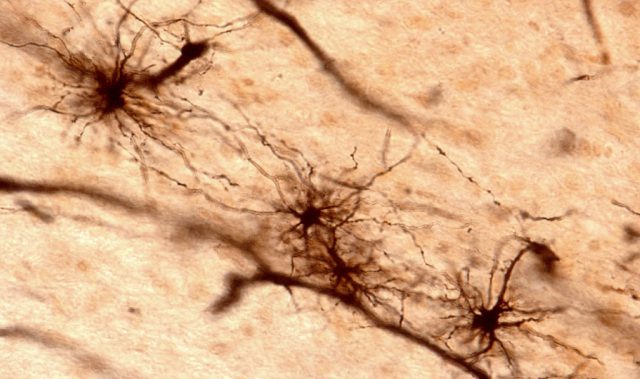
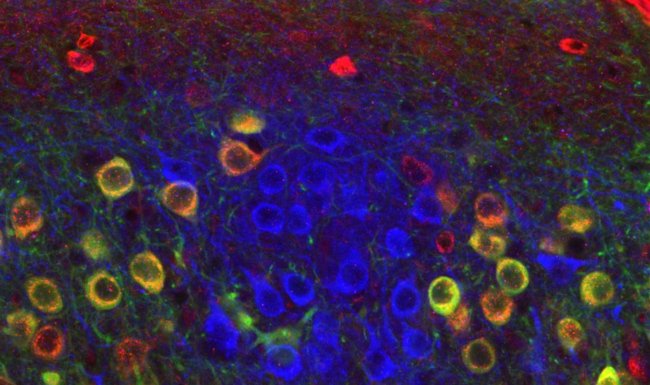
In the present study, scientist team discovered that reactive astrocytes in the brains of Alzheimer’s disease model mice produce the inhibitory transmitter GABA by the enzyme monoamine oxidase B (MAO-B). The reactive astrocytes then release GABA through the Bestrophin-1 channel to suppress normal information flow during synaptic transmission. Based on this discovery, the team was able to reduce the production and release of GABA by inhibiting MAO-B or Bestrophin-1, successfully ameliorating impairments in neuronal firing, synaptic transmission and memory in Alzheimer’s disease model mice.
In the behavioral test, the team used the fact that mice tend to prefer dark places. If a mouse experiences an electric shock in a dark place, it will remember this event and avoid dark places from then on. However, a mouse with modeled Alzheimer’s disease cannot remember if such shock is related to dark places and keeps going back to dark places. The team demonstrated that treating these mice with a MAO-B inhibitor fully restored the mice’s memory.
The drug selegiline is a MAO-B inhibitor that is currently used in Parkinson’s disease as an adjunct therapy. However, it has been previously shown to be less effective in Alzheimer’s disease. The team proved that selegiline is effective for a short time, but loses its efficacy in Alzheimer’s disease model mice in the long term. When treated for 1 week, selegiline brought the neuronal firing to a normal level. But when it was treated for 2 and 4 weeks, neuronal firing came back to the levels of untreated mice. From these results, the team proposed that there is a pressing need for a new drug that has long lasting effects.
Dr. Lee said, “From this study, we reveal the novel mechanism of how Alzheimer’s patients might lose their memory. We also propose new therapeutic targets, which include GABA production and release mechanisms in reactive astrocytes for treatment of Alzheimer’s disease. Furthermore, we provide a stepping stone for the development of MAO-B inhibitors with long lasting efficacy.”
The article can be found at: Jo et al. (2014) GABA from Reactive Astrocytes Impairs Memory in Mouse Models of Alzheimer’s Disease.
——
Source: Korea Institute of Science and Technology.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.