AsianScientist (Jun. 14, 2017) – Researchers from Japan have developed a stem cell-based therapy to treat a severe congenital bone defect known as myelomeningocele. Their findings have been published in Stem Cell Reports.
Myelomeningocele is the most serious and common form of spina bifida, a condition in which the backbone and spinal canal do not close before birth, leaving parts of the spinal cord and nerves exposed.
A baby born with this disorder typically has an open area or a fluid-filled sac on the mid to lower back. Most children with this condition are at risk of brain damage because too much fluid builds up in their brains. They also often experience symptoms such as loss of bladder or bowel control, loss of feeling in the legs or feet, and paralysis of the legs.
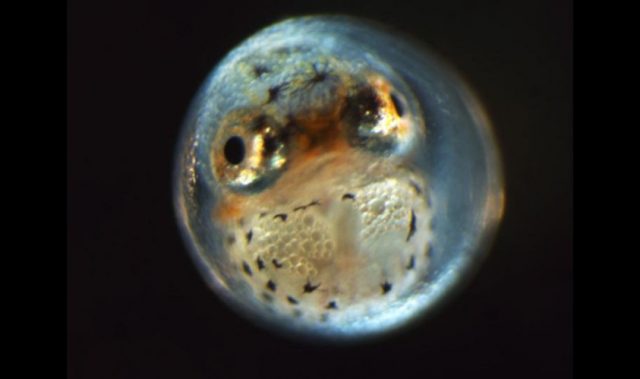
To develop a minimally invasive treatment to cover large myelomeningocele defects earlier during pregnancy, the researchers first generated artificial skin from human induced pluripotent stem cells (iPSCs), and then successfully transplanted the skin grafts into rat fetuses with the condition.
“We provide preclinical proof of concept for a fetal therapy that could improve outcomes and prevent lifelong complications associated with myelomeningocele—one of the most severe birth defects,” said senior study author Professor Akihiro Umezawa of Japan’s National Research Institute for Child Health and Development.
“Since our fetal cell treatment is minimally invasive, it has the potential to become a much-needed novel treatment for myelomeningocele.”
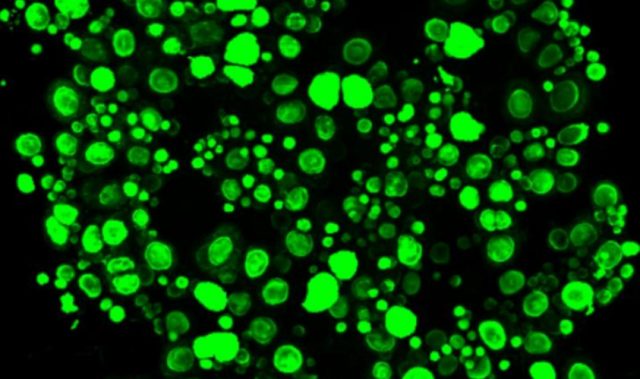
The human iPSCs were generated from fetal cells taken from amniotic fluid from two pregnancies with severe fetal disease (Down syndrome and twin-twin transfusion syndrome). The researchers then used a chemical cocktail in a novel protocol to turn the iPSCs into skin cells and treated these cells with additional compounds such as epidermal growth factor to promote their growth into multi-layered skin.
In total, it took approximately 14 weeks from amniotic fluid preparation to 3D skin generation, which would allow for transplantation to be performed in humans during the therapeutic window of 28-29 weeks of gestation.
Next, the researchers transplanted the 3D skin grafts into 20 rat fetuses through a small incision in the uterine wall. The artificial skin partially covered the myelomeningocele defects in eight of the newborn rats and completely covered the defects in four of the newborn rats, protecting the spinal cord from direct exposure to harmful chemicals in the external environment.
Moreover, the engrafted 3D skin regenerated with the growth of the fetus and accelerated skin coverage throughout the pregnancy period. Notably, the transplanted skin cells did not lead to tumor formation, but the treatment significantly decreased birth weight and body length.
“We are encouraged by our results and believe that our fetal stem cell therapy has great potential to become a novel treatment for myelomeningocele,” Umezawa said. “However, additional studies in larger animals are needed to demonstrate that our fetal stem cell therapy safely promotes long-term skin regeneration and neurological improvement.”
The article can be found at: Kajiwara et al. (2017) Fetal Therapy Model of Myelomeningocele with Three-dimensional Skin Using Amniotic Fluid Cell-derived Induced Pluripotent Stem Cells.
———
Source: Cell Press; Photo: Kazuhiro Kajiwara.
Disclaimer: This article does not necessarily reflect the views of AsianScientist or its staff.