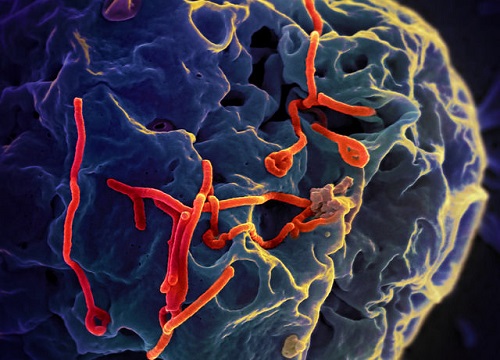
Asia must strengthen its defenses against the Ebola outbreak, urged World Health Organization (WHO) Director-General Dr. Margaret Chan. “In the simplest terms, this outbreak shows how one of the deadliest pathogens on earth can exploit any weakness in the health infrastructure,” she said in a meeting with health officials.
At the time of publication, the death toll from Ebola in 2014 has passed 4,500 people across seven countries, a figure that is still rising exponentially. With the battleground seemingly spreading out of West Africa, there is no doubt that Asia cannot afford to be on anything other than the highest alert.
Deep scars from SARS
To date, Asian countries have taken a pro-active role in the fight against Ebola, sending hundreds of trained healthcare workers, millions of dollars in donations, as well as protective gear and equipment to help with the West African outbreak.
With any luck, health systems across Asia will be able to contain the outbreak, should it occur, though it would not be their first brush with imported infectious disease: In the early 2000s, the region of 1.8 billion was ground zero for severe acute respiratory syndrome, or SARS.
The SARS coronavirus spread by air-borne respiratory emissions from Hong Kong to almost 40 countries, including China, Taiwan and Singapore, within weeks of its first appearance. In the ensuing outbreak, almost 1,000 individuals died, out of over 8,000 infected people.
Can biotechnology help us?
Because of the novelty of SARS, there were no vaccines, treatments or diagnostic tests available when the outbreak hit Asia. Ebola, in contrast, has been known for decades. In the 40 years since its discovery, there have been attempts at developing a biotechnology-based solution, but a lack of market demand has confined development to a few small academic or non-profit labs, and more recently, the vagaries of investment cycles.
On September 4, 2014, the share prices of US pharma company Chimerix plunged by more than nine percent on the NASDAQ stock exchange, despite jumping almost 40 percent in the last month. News had just broken that Thomas Duncan, a Liberian man who became the first person to be diagnosed with Ebola virus disease (EVD) in the US, had died. Physicians had been treating Duncan with brincidofovir, an experimental drug Chimerix had developed.
The few pharma companies already working on Ebola vaccines have also ramped up their development efforts. Some of these vaccines have entered human trials in the US, including one by pharma giant GlaxoSmithKine. Johnson & Johnson’s Crucell unit is currently working with the National Institute of Allergy and Infectious Disease (NIAID) on a modified human cold virus that carries Ebola genetic information. J&J’s vaccine is expected to start human trials this year.
Bracing for the worst
But a vaccine developed today could end up useless, scientists say, if the Ebola virus continues evolving as quickly as it has. A Broad Institute and Harvard University study published in the journal Science found that the 2014 Ebola strain has accumulated far more genetic mutations than seen previously.
In addition, determining if experimental drugs work is a challenge, because the current urgency in battling Ebola has necessitated that patients receive multiple interventions at the same time. In any case, the next steps to manufacture these medicines on a large scale won’t be cheap or easy.
The uncertainties of finding a drug or vaccine also highlight the importance of looking to other biomedical tools that can aid the Ebola effort. Researchers at Japan’s Nagasaki University have developed a polymerase chain reaction (PCR)-based detection test that only needs 30 minutes and a battery-powered warmer. If a blood or bodily fluid sample is positive for the Ebola virus, the solution turns cloudy, providing a simple tool that could prove a boon to healthcare workers in rural field hospitals.
“Given the rapid expansion of global travel in Asia and its economic development, Asia effectively will be connected to almost every part of the world,” Professor Leo Yee Sin, Director of the Institute of Infectious Diseases and Epidemiology at Singapore’s Tan Tock Seng Hospital told Asian Scientist Magazine.
“It is therefore vital for Asia to beef up its outbreak response within the region, improving outbreak research as part of its efforts. The scope of research in this area is wide, from research into the best detection methods to treatment, prevention and societal response.”
Pandemic preparedness
While Asia braces itself for Ebola, it should also be remembered that the next pandemic could strike from anywhere. Thankfully, the deep scars left by SARS and the more recent H1N1 and H7N9 bird flu scares have jolted Southeast Asian countries into action. The ASEAN Working Group on Pandemic Preparedness and Response is adapting a framework it developed from the SARS epidemic to fight the Ebola virus, should it prove necessary.
A good public preparedness framework is absolutely critical, but the right vaccine or drug could be the silver bullet that stops Ebola in its tracks. Right now, just a dozen or so biotech companies stand between us and Ebola. The failure to develop a working vaccine or treatment over the last 40 years raises the question of whether the development of much needed new therapies be left to market incentives. Given the potential for loss of life and economic devastation, this is a question that Asia cannot afford to ignore.
——
To read more, subscribe to Asian Scientist Magazine in print and receive four issues of Asian Scientist Magazine delivered directly to your mailing address for 12 months, inclusive of taxes and postage.